

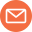

Psoriasis affects approximately 125 million people worldwide and is among the most psychologically and physically burdensome skin conditions a person can live with. The characteristic silvery plaques, chronic inflammation, unpredictable flares, and frequent inadequacy of topical treatments leave many patients feeling that their skin is an unsolvable problem. What most people with psoriasis have never been told is that their skin condition may be significantly driven by what is happening in their gut.
The skin is not merely an external barrier — it is a reflection of internal biological health. Chronic skin inflammation, whatever its specific diagnosis, represents an immune system in a state of excessive activation. Finding and addressing the upstream drivers of that immune activation — rather than suppressing skin inflammation topically — is the approach that produces genuine long-term improvement.
The gut is the upstream driver most frequently overlooked in chronic skin conditions. Research over the past decade has established clear biological connections between gut microbiome health, intestinal barrier integrity, and the immune dysregulation driving psoriasis and eczema.
The intestinal epithelium — the single-cell-thick lining of the small intestine — forms a selective barrier that allows nutrients to be absorbed while preventing bacteria, bacterial products, and incompletely digested food proteins from entering the bloodstream. The integrity of this barrier depends on tight junction proteins connecting adjacent epithelial cells, and on the short-chain fatty acids produced by beneficial gut bacteria that maintain tight junction function.
When gut dysbiosis depletes the beneficial bacteria producing these protective fatty acids, tight junction integrity is compromised, and the intestinal barrier becomes abnormally permeable — the condition colloquially known as leaky gut. This increased permeability allows bacterial lipopolysaccharides, microbial fragments, and food-derived antigens to pass into the systemic circulation, activating the systemic immune response that drives inflammation throughout the body — including the skin.
Multiple studies have documented distinct gut microbiome profiles in psoriasis patients compared to healthy controls. Psoriasis patients show reduced microbial diversity, depleted Faecalibacterium prausnitzii and other anti-inflammatory butyrate producers, and elevated populations of pro-inflammatory bacterial species. Importantly, the severity of gut dysbiosis correlates with psoriasis severity — greater microbial imbalance is associated with more extensive and more refractory skin disease.
The mechanism connecting gut dysbiosis to skin inflammation involves multiple pathways. Gut-derived bacterial endotoxins entering the bloodstream through a leaky gut activate Toll-like receptor 4 on immune cells, triggering the TNF-alpha and interleukin-17 inflammatory cascades that are central to psoriatic skin inflammation. The very inflammatory mediators targeted by the most advanced biologic psoriasis treatments are being chronically activated by gut-derived bacterial signals in patients with significant gut dysbiosis
The gut-skin connection is equally well established in eczema. Research in infants demonstrates that gut microbiome composition in the first weeks and months of life predicts eczema development, with early Lactobacillus and Bifidobacterium colonisation providing protective effects through immune programming. Disrupted infant microbiome development — from caesarean birth, formula feeding, or early antibiotic exposure — is among the most consistent risk factors for childhood eczema.
In adults with eczema, gut dysbiosis drives skin inflammation through IgE sensitisation facilitated by increased gut permeability, systemic mast cell priming from gut-derived histamine and inflammatory mediators, and impaired immune tolerance from dysbiotic disruption of regulatory T cell function.
IgG-mediated food sensitivities — common in individuals with compromised gut barrier function — drive chronic skin inflammation through immune complex deposition in skin capillaries and the sustained immune activation of repeatedly consuming reactive foods. Many individuals with psoriasis and eczema find significant symptom improvement when IgG food sensitivity testing reveals their specific reactive foods and elimination reduces the immunological load driving their skin inflammation.
A root-cause approach to psoriasis and eczema begins with comprehensive gut microbiome assessment revealing the specific dysbiotic patterns present, food sensitivity testing identifying immunologically reactive dietary triggers, and intestinal permeability assessment quantifying the barrier compromise driving systemic immune activation. Together, these investigations provide the biological roadmap for a targeted treatment plan that addresses the gut origin of skin inflammation.
Your psoriasis or eczema is not simply a skin problem — it is a systemic immune condition with its roots frequently embedded in gut microbiome health and intestinal barrier function. Addressing the gut biology driving your skin inflammation offers a genuinely root-cause approach that conventional topical management cannot provide. The clearest path to clearer skin may run directly through your gut.
Written by: Dr. Bakshi's Advance Diagnostics Team
Reviewed by: Certified Health Experts
Published: April 2026
This article is written and reviewed by the expert team at Dr. Bakshi's Advance Diagnostics, specializing in advanced diagnostic testing including gut health, food intolerance, and genetic testing.